INEC releases 2019 election timetable, interdicts 23 Rivers rerun officials
January 12, 2018
Book Review: A Life called Forever
January 12, 2018
By Oghenechovwen Oghenekevwe
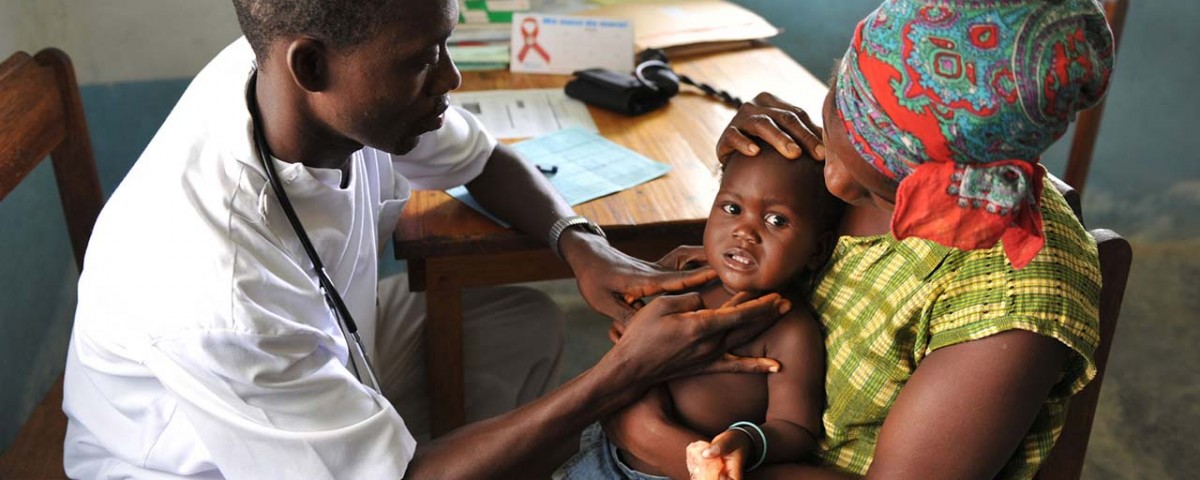
Beautiful, patterned white lines and detailed symbols traced the walls of the room. Inside there, in Gbolaka-Ta village, young Liberian girl Hawa Singbeh almost died from Ebola in 2015 – the same room she was born in. Her brother and sister did not survive this virus.
The most complex and widespread Ebola virus disease outbreak in history occurred in six West Africa nations, from 2013 to 2016. Ebola, which spreads by contact with body fluids of infected humans and handling or eating infected primates, is a violent haemorrhagic fever that leads to internal and external bleeding and organ failure.
Data from World Health Organization tells us that the “Ebola epidemic claimed the lives of more than 11, 300 people and infected over 28, 500” in Liberia, Sierra Leone, Nigeria, Mali, Senegal, and Guinea. Under a rapid-containment scenario, West Africa’s estimated GDP lost to Ebola by 2015 was $1.6 billion. In Sierra Leone alone, federal authorities said the impact resulted in an economic deflation by 30 percent.
Ebola is not the end of reality. There are other dreadful viruses that are now increasingly upon us, especially in West Africa. Lassa fever, Meningitis, and Monkeypox are sad viral examples. Decades after their respective index cases in this tropical region, virus diseases are now remerging in epidemic proportions.
For example, Nigeria last year experienced deadly outbreaks of Lassa fever, meningitis, and Monkeypox. Monkeypox is a rare disease that largely resolves itself (no specific treatment or vaccine available), and has milder symptoms in humans similar to those previously manifested in smallpox patients. In 1971, there were two Monkeypox cases in Nigeria. And only a single case was recorded seven years after. The Nigeria Centre for Disease Control, in October 2017, confirmed a total of 94 cases from eleven states and the Federal Capital Territory.
When one goes far beyond superficial observation on how these increasing viruses are spread and their season of occurrence, real associations between rising global temperatures, human-animal proximity, and public health effect can be documented.
In a 2015 research paper published in Science and co-authored by 18 leading scientists and stakeholders, Johan Rockström reveals that humanity has sprinted past four out of nine “planetary boundaries” – crucial limits for keeping earth stable and hospitable. People are forcing earth into uncertain and dangerous territory – driving up global temperatures, clear-cutting original forests, dumping fertilizers into rivers and oceans and forcing animals, plants and other organisms towards extinction. Rockström, who had the idea of planetary boundaries back in 2007, is executive director at the Stockholm Resilience Centre.
Today’s numbers on the state of the planet shows that carbon dioxide (an important greenhouse gas that causes climate change) levels are unsafe at 400 parts per million and climbing, 16 percent of biodiversity has been lost around the world, and instead of conserving at least 75 percent of forests, only 62 percent are left due to deforestation and other land use changes.
Will Steffen, the paper’s lead author, believes that crossing the boundaries of climate change and the health of the planet’s ecosystems is troubling since doing so “can shove the earth into completely different states”. Steffen is also the executive director of the Climate Change Institute at the Australian National University.
My experience during the first Online Youth Exchange of Care About Climate and the China Youth Climate Action Network helped put the impact of climate change on public health and biodiversity in context. It was a one-year international capacity building programme and, like other participants, I had to give a webinar. Mine was on climate change and its intersection with viral diseases in West Africa. Here is what I learnt while prepping.
We have an underreported climate crises in parts of West Africa: areas off the Abidjan harbor experience high soil erosion rates and loss of mangrove swamps; resulting surface floods from heavy rainfalls and rising sea levels are disrupting the lives of waterfront dwellers in Lagos islands; neighbouring settlements of the Ivorian western, land boarders with Liberia and Guinea are now seeing changes in ecosystems; and the availability and quality of Sierra Leone’s extensive water resources is significantly challenged as a result of shortages, intense sediment loads, and temperature-driven microorganism reproduction cycles and algal growth, thus, providing more conducive breeding grounds for disease vectors – up to 80 percent of the country’s rural population obtains its water from these sources.
Often in this massive region, deforestation is on the rise, warming events are enduring, and vegetative covers are changing. The number of young people is getting bigger and bigger and so takes this climate crisis downhill. Yet, there is no concerted, scientific research effort to evaluate and understand the impacts of this crisis on ecosystems and human systems, particularly habitats fragmentation and public health.
Perhaps, public health is the most unevaluated human face of climate change. And compelled by warming and instability, our climate is playing a tremendous part in perpetuating the global emergence, resurgence and spread of infectious diseases.
Most infectious diseases have three components: a pathogen, a host, and a transmission environment. Some viruses are pathogens since they are examples of disease-producing agents. Host refers to living animal or plant that supports and nourishes disease pathogens. While transmission environment involves the indirect and direct distribution or spread route of disease.
A 2002 study published in Science shows that temperature can influence the reproduction and development of pathogens. According to Dr. Aaron Bernstein, Centre for Health and the Global Environment scholar at Harvard University, “all pathogenic viruses…and parasites are temperature sensitive.” For example, coinciding with the Ebola outbreak in West Africa, global temperature in the months of May had anomalies from 2014 up to 2017. Put simply by Goddard Institute for Space Studies at the National Aeronautics and Space Administration (NASA), each May in these years were the top 3 hottest in 137 years of modern, global temperature record–keeping.
The biggest misconception about climate change is that everything, everywhere gets warmer. However, it is necessary to know that temperature change over land and water may or may not restrict the development and distribution of viral diseases. This depends on their distinctive temperature thresholds.
_____
Have you also read?
PBR Cowpea could generate N48 billion for Nigeria
_____
Furthermore, extreme positive shifts in rainfall amount – often driven by climate change – plays a quiet role in the development of select disease pathogens, as continuous, heavy rain may mix sediments in water and land upwards, leading to the accumulation of fecal microorganisms at surface levels.
Human-animal proximity and close interaction are also likely to support the development, survival, and redistribution of infectious diseases. In this case, intermittent connections of these diseases with wildlife, extreme weather events, and meteorological hazards are seen.
Jungles and deep, unexplored areas are sometimes the natural reservoirs of an infectious disease or the habitat of host animals. People are pushed to these areas from their original homes; as a result of droughts, famines, heatwaves, and floods; for survival and in pursuit of favourable living conditions. When we migrate to these areas, we deforest to commercially farm cash crops, site manufacturing industries, construct roads, and so on.
We alter the habitats of reservoirs and hosts. During hazards, for example, rodents that hosts Lassa virus may enter homes to look for food and transmit it to humans, leading to Lassa fever cases. In peri-urban populations of low-income countries, the risk factors for Swamp fever include flooding of open gutters and streets.
“Rising global temperatures would have a catastrophic effect on human health and patterns of infections will change”, Nigeria’s Federal Minister of Environment, Usman Jubril, says.
But we can lessen the extent of this foreseen, catastrophic effect.
Through academic research and science-based methods to meaningfully understand the impacts of climate change (including extreme weather events and meteorological hazards) on public health, especially viral diseases; investing more in surveillance, monitoring and early warning systems; practising open information and experience sharing; and building the capacities of vulnerable populations via campaigns and outreaches, we can help deliver a healthier and sustainable tomorrow for Hawa Singbeh. For everyone.
___________
Oghenechovwen Oghenekevwe studies Meteorology and Climate Science at The Federal University of Technology Akure, Nigeria. His creative stories focus on human and social topics, and how they often interrelate with our shared environment. Follow him on twitter: @ChovwenKevwe
(Image Credit: Guardian)
Disclaimer: The opinions expressed in this article are those of the author not of NDLink